
Startup harnesses AI to improve ICU patient care
Leon DeJournett, M.D., chief medical officer and founder of Ideal Medical Technologies in Asheville, N.C., has been leading the development of an innovative technology for controlling blood sugar (or glucose levels) of patients in the intensive care unit (ICU). The company’s FUSION system has already demonstrated exciting positive results in its first clinical trial.
“By offering safe and effective glucose control, we think our hospital-based system could save up to 200,000 lives per year in the ICU setting,” said DeJournett. “It could also potentially decrease healthcare costs by 5 to 10 billion dollars a year in the U.S. alone.”
The company has been awarded loan funding from the North Carolina Biotechnology Center to support system development, laboratory testing and clinical testing. This loan supplements a two-year $1.9 million Phase II Small Business Innovation Research (SBIR) grant the company received from the National Institute of Diabetes and Digestive and Kidney Diseases in 2022.
"We are excited not only about the potential that Ideal Medical’s FUSION system could have on health outcome in hospitals, but also the value that hospitals could receive by freeing up nursing time through automation and the potential reduction of health care worker burnout," said Mike Carnes, vice president, Emerging Company Development, NCBiotech.
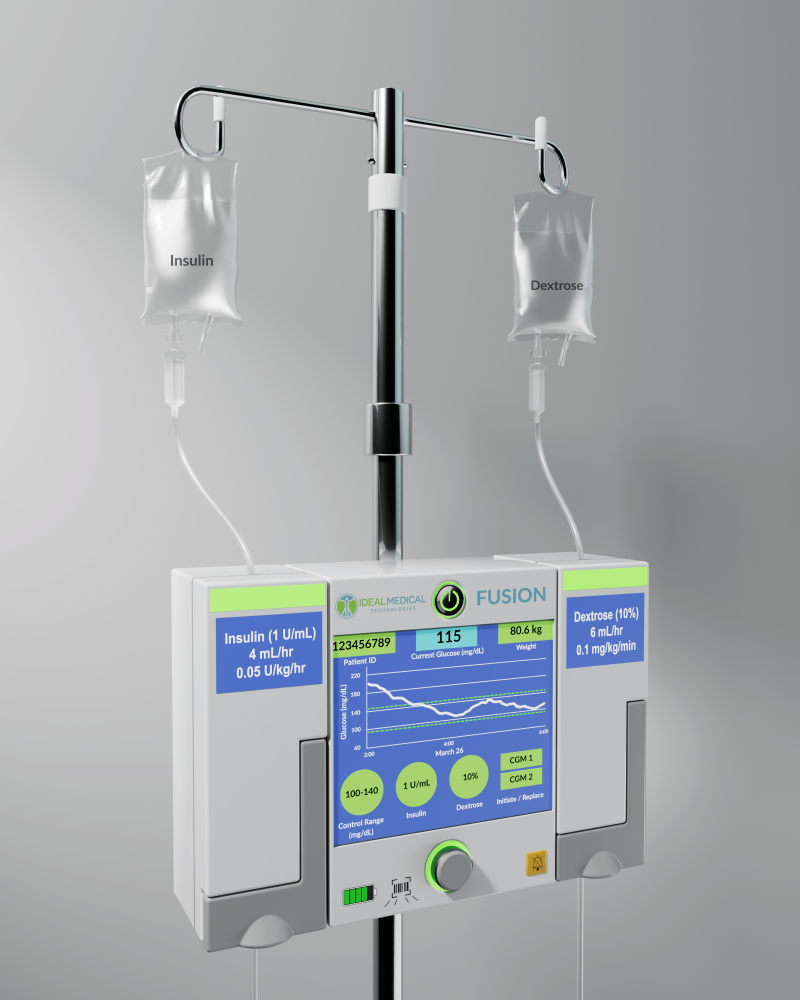
To develop the FUSION closed-loop glucose control system, DeJournett combined his experience with treating children with type 1 diabetes in the pediatric ICU with his team’s electrical engineering and computer programming expertise. The automated system uses AI algorithms that DeJournett developed to mimic the body’s natural systems, enabling highly automated control of blood glucose levels without the need for frequent interventions from health care staff.
Why is blood sugar so important?
When someone is in the ICU, their body is under a great deal of stress. Even for patients without diabetes, this stress can raise blood sugar levels enough to trigger a cascade of inflammatory markers that contributes to increased morbidity and mortality rates. Studies have shown that using IV-administered insulin to control blood sugar levels for ICU patients can lower morbidity and mortality rates by up to 30 percent to 40 percent and shorten the overall hospital stay by 1-2 days, which can reduce healthcare costs by at least $3,000 per ICU patient.
However, current blood glucose control procedures in the hospital setting are a very labor and time-intensive process. They require nurses to prick the patients’ fingers to take glucose readings, enter these glucose values into insulin dosing software, and based on the software’s recommendations manually adjust the patient’s intravenous insulin infusion pump. This process may be repeated as frequently as every 1-2 hours, is prone to human error at each step, and can take up to 2 hours of nursing time per patient per day to complete. Even then, the body’s blood sugar changes minute-to-minute, especially when stressed, so this method doesn’t always produce the best results.
The FUSION system, which looks like a traditional IV pump commonly found in the hospital, uses insulin to lower blood sugar and dextrose (IV glucose) to raise blood sugar in what is known as a two-bag system. Using AI, the system automatically adjusts infusion rates of intravenous insulin and dextrose every 5-10 minutes based on readings from a commercially available continuous glucose monitor (CGM). The FUSION’s fully autonomous system not only reduces the time that nursing staff must spend on this critical function, but also has the potential to do a better job at keeping glucose levels within a safe range as compared to the currently used highly manual approach.
Who could benefit?
Studies have shown that ICU patients without diabetes tend to experience more negative effects from high glucose levels than those with diabetes, so this group of ICU patients, which accounts for 70 percent of all ICU patients, would benefit most from the new system. In addition, the FUSION system is also being developed to stabilize blood sugar levels of diabetic patients in both the ICU and non-ICU settings.
“ICU patients and patients with diabetes in the non-ICU setting make up about 40 to 50 percent of all hospitalized patients,” said DeJournett. “This equates to 14-15 million patients a year in the U.S.”
After conducting successful simulation and animal studies with the FUSION system, the company completed its first human clinical trial in 2023 with support from a loan received from NCBiotech in 2021. The company worked with experts in inpatient glucose control at Emory University to perform a proof-of-concept safety study on patients with type 1 and 2 diabetes in a simulated ICU setting.
The system worked very well, demonstrating the ability to keep patients in a healthy blood glucose range between 70-180 mg/dL 88 percent of the time with no instances of dangerous low blood sugars in 24-hour unannounced meal challenge studies. These studies simulate real-world scenarios where individuals with diabetes might consume meals without prior planning.
What’s next?
During the first part of 2024, the company plans to translate its prototype system into a commercial-grade system. The company plans to complete human clinical trials by early 2026 and is aiming to have an FDA-approved device within the next three years.
Although Ideal Medical Technologies is focused on glucose control right now, its custom-built intravenous pump platform could potentially bring fully autonomous control to other areas of ICU care. These include control of blood pressure levels; blood osmolality levels, which are important for brain trauma and stroke patients; blood volume status, which is important for trauma and sepsis patients; and automated dosing of intravenous antibiotics.
“We are working to create a platform system that automates a lot of the bedside care in the ICU setting, which will improve nursing efficiency,” said DeJournett. “This is very important given the current nursing shortage being experienced throughout U.S. hospitals.”
