
NC Biotechs: Overcoming Resistance to Developing Antibiotic Resistant Therapies
U.S. Senator Todd Young (R-IN), who has co-led a bi-partisan Congressional effort to address the issue, points out that the pipeline for antibiotics remains “woefully insufficient. Without swift and comprehensive action to spur urgently needed innovation,” he warned, “we may soon find ourselves in a post-antibiotic era, when even a simple medical procedure could be deadly.”
As big pharma has largely moved away from antibiotic development over the past couple of decades, small and midsized biopharmaceutical companies have stepped into the breach. That includes North Carolina startups FleurirABX, RAIN Scientific, Locus Biosciences and Resilient Biotics.
They, and other companies like them, face significant challenges. If they fail, the threats to modern medicine are real and potentially severe. But there is hope on the horizon, and optimism that new treatments are on the way.
Penicillin and the dawn of the golden age of antibiotics
When 73,000 U.S. troops landed on the beaches of Normandy on D-Day, they carried with them millions of doses of penicillin – a brand-new miracle drug.
The antibiotic is credited with helping save the lives of more than 100,000 men in the European Theater between D-Day on June 6, 1944, and the final German surrender on May 7, 1945.
Contrast that with the experience of World War I, where about half of the 10 million soldiers who died weren’t killed by bullets, bayonets, or bombs, but by untreatable infections that developed from often minor wounds and other injuries.
The modern era of antibiotics started with Sir Alexander Fleming’s discovery of penicillin in 1928, first commercially developed and manufactured in the 1940s to treat bacterial infections among World War II soldiers. It was made available to the general public in the United States in 1945.
The drug’s tremendous success soon became its biggest liability. Its broad use, overuse and misuse caused penicillin resistance to become a serious clinical problem only a decade after the drug was launched. It was a concern Fleming himself had raised in 1945.
But other classes and variations of drugs soon followed during what’s been called the golden age of antibiotic discovery, from the 1940s to the 1960s. The big problem is that whenever new antibiotics are introduced, resistance to them will invariably develop – sooner or later. So there is a constant battle to come up with new and better treatments to attack the superbugs that have successfully adapted to older therapies.
High development costs, low returns discourage antibiotic investment
That’s where the rub comes in. Since the 1970s, the antibiotic pipeline has narrowed considerably as large pharmaceutical companies have – for the most part – abandoned development because the economics don’t support their efforts. No new classes of these drugs have been discovered since the 1980s.
Big pharma has chosen instead to focus on chronic conditions requiring long duration therapies that sell at higher prices. That’s left small and mid-sized biotech companies to fill the gap – they now account for close to 95% of the antimicrobial drugs developed. But they often lack the financial clout to shepherd new medicines all the way from discovery through market approval and launch.
Research and development is difficult, expensive and time consuming. It can take a decade or two and an investment of more than $1 billion to introduce a new antibiotic, and the failure rate is high.
Yet these medicines are sold for relatively low prices compared to cancer treatments and many other therapies that manage persistent diseases. And, because newer antibiotics are considered drugs of last resort to treat dangerous bacteria, doctors prescribe them sparingly and for shorter periods of time to delay the onset of drug resistance.
High investment costs – coupled with comparatively modest returns, lower potential sales and challenging regulatory requirements – make it difficult to break even, let alone turn a profit. Add to that the dearth of private funding available to support the development of these medicines.
Achaogen and Melinta – two small antibiotics producers – are a case in point. Both filed for bankruptcy in 2019 even though each company had received U.S. Food and Drug Administration approval and brought a new antibiotic to market.
Marketplace dynamics have contributed to a global antibiotic – or antimicrobial – resistance (AMR) crisis. The U.S. Centers for Disease Control and Prevention estimates that close to three million AMR infections occur in this country each year. These illnesses kill someone every 15 minutes – resulting in around 35,000 deaths annually.
Worldwide, the death rate is at least 1.7 million, a number that could increase to 10 million a year by 2050, according to a report commissioned by the UK government.
“The times they are a changin,” as biotechs explore new AMR treatments
But, to borrow a line from singer/songwriter Bob Dylan, “The times they are a-changin” – albeit slowly.
Governments and other organizations are beginning to look for more innovative ways to encourage antibiotic development by removing some of the financial and regulatory hurdles. This paradigm shift is not coming any too soon.
“Antibiotic resistance threatens modern medicine as we know it,” Senator Young has said, “but the U.S.’s current level of preparedness does not match the magnitude of the threat.”
He and Senator Michael Bennet (D-CO), along with House members Mike Doyle (D-PA) and Drew Ferguson (R-GA), are cosponsoring the Pioneering Antimicrobial Subscriptions to End Upsurging Resistance – or PASTEUR – Act of 2021. The legislation, if passed, will create market incentives to develop new, lifesaving antibiotics.
Despite the sizeable challenges, and as more attention is directed at the crucial need for new antimicrobial therapies, North Carolina’s biopharmaceutical industry is working to fill the void. Home grown companies are helping lead the way to what many hope will be another productive era of antibiotic development. Here are a few notable examples.
FleurirABX combines old drugs to create new, more powerful antibiotic
FleurirABX, a Raleigh-based specialty pharmaceutical start-up, is teaching two old dogs new tricks with its synergistic combination antibiotic, FTS.

The company takes advantage of convergent metabolic pathways within bacteria to find better drugs to treat bacterial infections. By combining the right compounds, FleurirABX can develop more powerful products to treat a wider range of pathogens more effectively and reduce the bacterial resistance that inevitably develops.
The company has combined two older drugs, Fosfomycin (F) and trimethoprim-sulfamethoxazole (TS), to create a powerful and broader-spectrum antibiotic that is much less susceptible to AMR. FleurirABX said it has patented FTS in the United States, Mexico, and Taiwan, with other patents pending.
The project is the most advanced in the company’s portfolio. FTS is more potent than either of the individual antibiotics it is made up of – according to FleurirABX – and can be administered both orally and intravenously.
Both fosfomycin and trimethoprim-sulfamethoxazole have been on the market for decades and have excellent safety profiles, which could reduce the amount of new data needed for regulatory approval, according to John Pace, Ph.D., the company’s vice chairman and chief scientific officer.
He said the combination’s emerging profile suggests that it could be ideal for treating urinary tract and both gram-positive and gram-negative infections, replacing standard therapies. Importantly, it can kill both aerobic and anaerobic bacteria.
The company is securing the funding necessary to collect more scientific evidence to support the safety and effectiveness of FTS.
FleurirABX was founded in 2013. In addition to Pace, who is co-inventor on 20 U.S. patents, the company’s executive team includes Steven Volla, chairman and CEO, and Susan Gardlik, Ph.D., chief operating officer.
RAIN Scientific develops medical device that targets AMR

RAIN Scientific is working closely with the U.S. Department of Defense on a non-pharmaceutical antimicrobial therapeutic called GENESYS.
It consists of an intravenously placed device worn continuously for a specific amount of time that is determined by the pathogen it is treating and other factors. RAIN co-founder and CEO Tim Koehler said data collected so far indicate that disease-causing microorganisms aren’t likely to develop a resistance to the technology.
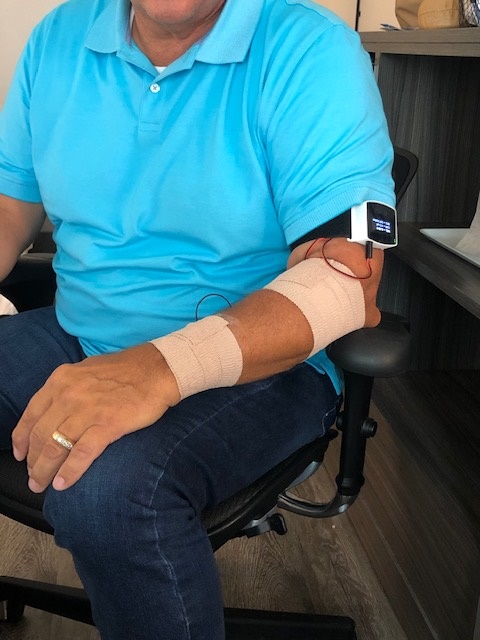
The startup biotech, founded in 2017, has completed extensive in vitro (outside living organism) studies that have shown its technology can safely stop the growth of gram-positive and kill gram-negative bacteria. Additional research, combining GENESYS with standard-of-care antibiotics to attack bacterial resistant infections, is underway in both in vitro and small animal in vivo (living organism) studies, Koehler said.
The company also plans to conduct its own in vivo porcine blood model to measure GENESYS’ effectiveness against sepsis, a life-threatening condition that occurs when the body’s immune system overacts to infection and starts to damage tissues and organs.
Koehler said RAIN will evaluate the product’s safety and effectiveness over the next 24 months and be ready to market GENESYS within 36 months. The company hopes to license the technology to a larger biotechnology or pharmaceutical company to treat blood stream infections.
RAIN’s other co-founders include Mike Davis, MD, the company’s chief medical officer, and Rodney Chan, MD, chief scientific officer. Both Davis and Chan have extensive high level military medical experience.
RAIN Scientific is headquartered in Huntersville, just outside Charlotte.
Locus deploys bacteriophage technology to attack superbugs
Morrisville-headquartered Locus Biosciences is developing a new version of its engineered bacteriophage technology to tackle antibiotic-resistant superbugs.

The company’s “smart bomb” therapies are designed to selectively kill targeted disease-causing bacteria, while leaving good bacteria in the body unharmed. Bacteriophages, or phages, hijack the bacterium’s cellular machinery to stop it from producing bacterial components.
In January 2019, Locus inked a contract with Janssen, the pharmaceutical arm of global powerhouse Johnson & Johnson. The goal is to develop engineered bacteriophage products targeting two of the most prominent bacterial species linked to muti-drug resistant infections – Pseudomonas aeruginosa and Staphylococcus aureus. The contract will provide Locus with up to $818 million in upfront and milestone payments, along with royalties on product sales.

Two years ago, the company signed an agreement with CARB-X (Combating Antibiotic-Resistant Bacteria Biopharmaceutical Accelerator) to help fund its investigational product to treat recurrent urinary tract infections (UTIs). Locus also plans to develop the therapy for lung, intra-abdominal and bloodstream infections.
CARB-X is a global non-profit that supports research and development to address the rising threat of drug-resistant bacteria. It is providing Locus with up to $12.5 million in funding.
Locus also has received support from the Biomedical Advanced Research and Development Authority (BARDA), a unit of the U.S. Department of Health and Human Services, for another investigational product designed to treat UTIs caused by E. coli bacteria.
BARDA is providing about half the $144 million needed to fund Phase 2 and Phase 3 clinical trials.
Locus’ engineered bacteriophage technology is unique. It combines two mechanisms of action – the bacteria-killing capability of the phage itself, along with engineered payloads that shred target DNA and cause cell death. This one-two punch helps tackle drug resistance. It’s a potentially powerful tool that can attack a variety of different infections.
The company got its start in 2015 as a North Carolina State University spin-out. The North Carolina Biotechnology Center helped support its early development. Paul Garofolo, one of Locus’ four co-founders, is CEO.
Resilient Biotics uses microbiome to reduce reliance on antibiotics
Resilient Biotics is taking a different approach focused on livestock.

The Research Triangle Park-based startup has built a drug discovery platform that targets the microbiome, the community of microorganisms that exist in various parts of the body. The idea is to develop microbiome-based products that promote respiratory health, prevent pathogens from taking hold of the respiratory tract, and reduce antibiotic dependence.
The company’s co-founder and CEO Christopher Belnap, Ph.D., said Resilient currently is working on an antibiotic-free nasal spray to prevent bovine respiratory disease (BRD).

BRD is among the most common causes of illness and death in cattle. Resilient’s nasal product works like a human probiotic to help cows’ respiratory systems maintain a healthy community of organisms while it strengthens immune response.
“We can use our technology to identify and help prevent the establishment and growth of pathogens that cause respiratory infections,” Belnap explained. “It’s a brand-new approach; there’s nothing like this on the market.” He said preliminary data support the product’s safety and effectiveness.
Antibiotics, the current treatment of choice for BRD, also are used proactively to prevent livestock diseases. Resilient’s new product could change that pattern, creating a dual positive effect. It would limit the possible development of antibiotic resistance in herds. And – with 70-80% of the total U.S. volume of antimicrobials sold for farm use – it could help lessen concerns that antibiotics transmitted to humans through the food they eat are increasing the likelihood of AMR.
Resilient also is exploring potential products for swine and poultry. Belnap thinks the technology has applications for human health, as well. He said the startup is expanding its research and development team and has recently partnered with a large company to continue to develop its BRD therapy. Product approval, if all goes well, is expected in three to five years.
Resilient Biotics was co-founded in 2017 by Belnap, a microbiologist. Rachelle Galvin, a Ph.D. pharmacologist and industry veteran, is president and chief operating officer.
“The work of these small and mid-sized North Carolina biopharmaceutical companies is more and more important as antibiotic resistance continues to spread both in the U.S. and in other countries around the world,” said Vivian Doelling, Ph.D., the North Carolina Biotechnology Center’s vice president of Emerging Company Development. “They can play a vital role in creating the new therapies that are so important to preventing infection and slowing AMR.”
What will the future look like?
While the biotech sector is making steady progress in its quest to find new solutions to address antibiotic resistance, will these efforts be too little and come too late? Will governments and other investors provide the incentives and financial support needed today to develop the antimicrobial therapies of tomorrow?
“Whether we’re going to succeed before the next crisis comes along is the question mark,” said Sue Gardlik of FleurirABX. “Or will we see huge treatment gaps and lots of people die over decades before anything happens to broadly address the problem,” added her colleague, John Pace.
One thing is certain – there’s no easy or quick way to fix the AMR crisis.
“Microbes have been creating and defeating antibiotics for billions of years,” wrote physicians Brad Spellberg and David Gilbert in an article for Clinical Infectious Diseases. “In contrast, in just 80 years of clinical use, humans have so abused antibiotics that we threaten their availability for future generations.”
But companies in North Carolina and elsewhere that are developing the next generation of antimicrobial therapies offer hope that help is on the way.
